Asthma & The Gut Microbiome ~ The Gut-Lung Axis
Asthma & The Gut Microbiome ~ The Gut-Lung Axis
Hippocrates, the Greek physician regarded as the “Father of Medicine,” is well known for his proclamation that “all disease begins in the gut” over two thousand years ago. In 2026, we now know that his astute words are correct as we continue to learn how the gut microbiome and gut microbiome metabolites play a critical role in the prevention and pathology of many chronic diseases, including pulmonary diseases such as asthma.
Yes, gut health affects lung health!
 Asthma Symptoms, Risk Factors & the Gut Microbiome-Lung Axis
Asthma Symptoms, Risk Factors & the Gut Microbiome-Lung Axis
Emerging experimental and epidemiological evidence confirms there is crucial crosstalk between the gut microbiome and the lungs. When the gut microbiome changes due to diet, antibiotic use, or other factors, the airways in the lungs could be affected. Fortunately, there are healthy practices that you can recommend to your patients to support the optimal function of both the gut microbiome and the lungs.
It is estimated that asthma currently affects over 300 million people worldwide. Some of the risk factors that can contribute to the development of asthma during childhood or adulthood include prenatal and early-life stress, delivery by cesarean section, genetics, use of antibiotics during the neonatal period, a maternal diet low in fiber, milk formula feeding, gender, ethnicity, monthly household income, higher BMI, smoking status, exposure to air pollution, and the diversity of microbes in the microbiome.1-3
Asthma is a chronic inflammatory disease characterized by symptoms that include wheezing, cough, shortness of breath, and chest tightness.4 Since asthma is caused by inflammation, treatment options focus on reducing inflammation or minimizing the effects of the inflammation. While those with asthma must keep at least one emergency medication on hand at all times, there are natural treatment options that could reduce inflammation and the symptoms of asthma. For example, research suggests consuming more fruits and vegetables is associated with fewer asthma symptoms.5 Research also shows the gut microbiome has a profound effect on the lungs, so nourishing and balancing the gut microbiome could reduce inflammation to improve the health of the lungs.1
What is Gut Microbiome Dysbiosis?
The typical healthy patient has trillions of microorganisms distributed throughout the entire gastrointestinal tract, and they are collectively referred to as the gut microbiome. Several large research studies, including the Human Gut Microbiome Project and the Human Microbiome Project, have provided insight into the composition of the gut microbiome. Ongoing investigations continue to reveal the numerous beneficial effects a healthy gut microbiome exerts on human health.6
Research shows the bacteria and other organisms present in the gut microbiome do affect respiratory health, and the phenomenon is known as the “gut-lung-axis.” While we know a healthy gut microbiome provides health benefits, it is important to acknowledge that an unhealthy or imbalanced gut microbiome can contribute to disease.1 When the organisms in the gut microbiome are not in optimal balance, it is known as dysbiosis. Dysbiosis is associated with the development of several chronic diseases, including allergies and asthma.1
Several studies confirm dysbiosis of the gut microbiome early in life leads to an enhanced risk for asthma development.6,7 Furthermore, the administration of gut microbiota from healthy neonatal mice protects against the development of allergic airway inflammation in germ-free mice without microbiota.8 Thus, inflammation or imbalance in the gut microbiome does appear to directly contribute to lung inflammation, according to the latest research.6
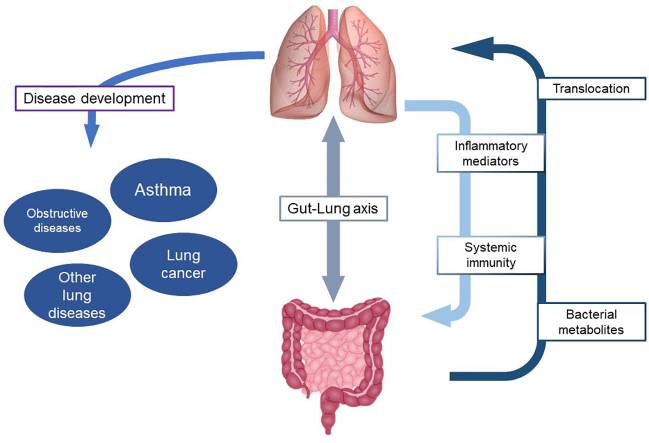 Image Source: Editorial: Innate immunity and severe asthma: From microbiome to target therapy – PMC
Image Source: Editorial: Innate immunity and severe asthma: From microbiome to target therapy – PMC
How Does the Gut Microbiome-Lung Axis Affect Pulmonary Health?
Hundreds, potentially thousands, of metabolites are produced by the gut microbiome. The gut microbiome metabolites then circulate systemically to distant organs, including the lungs.9 The metabolites produced by the gut microbiome are considered postbiotics, a relatively new area of research. Postbiotics were only recently defined in 2021 by the International Scientific Association of Probiotics and Prebiotics (ISAPP).10
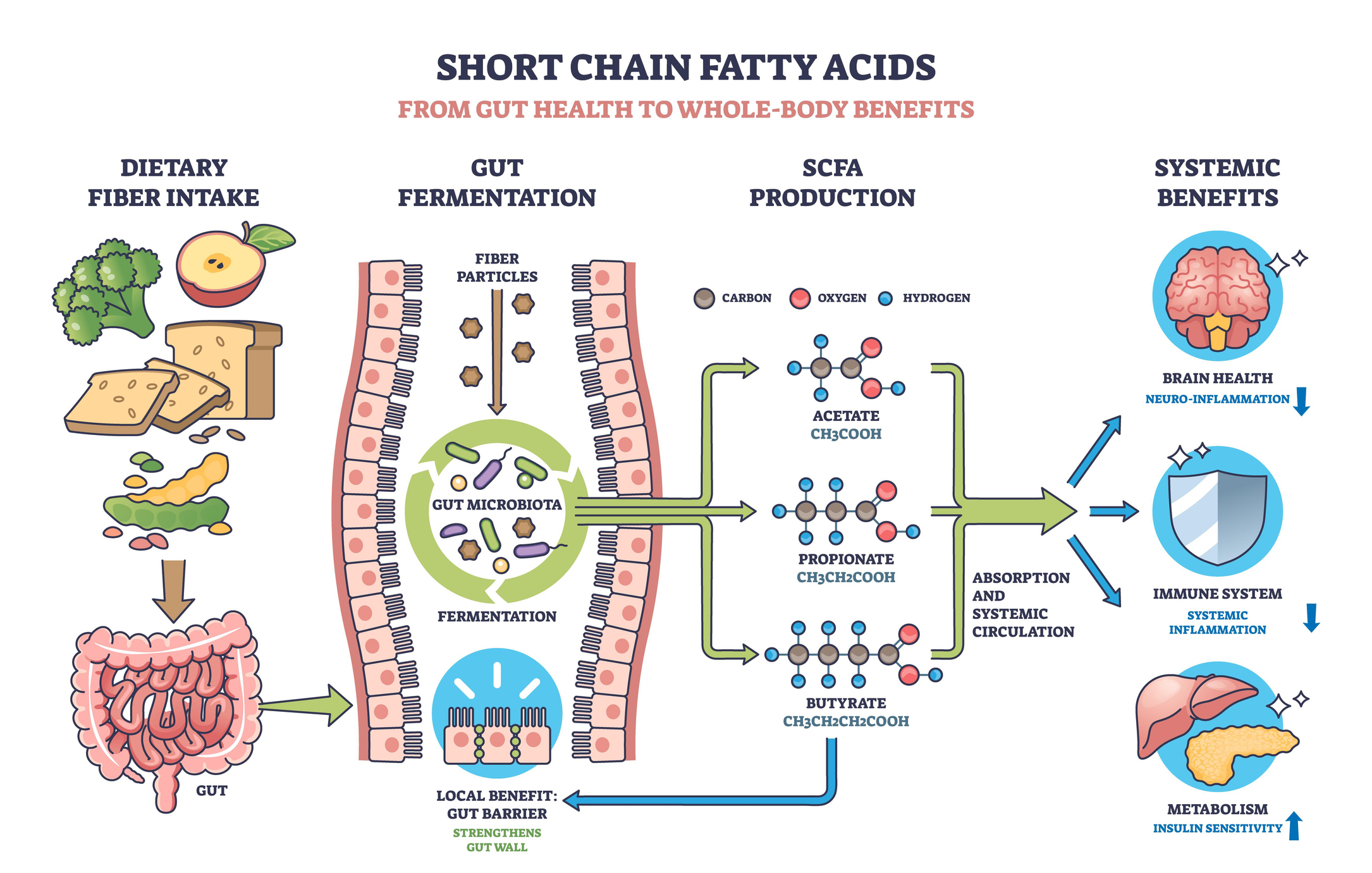
Even though postbiotics are a relatively new research topic, the results of the studies are quite exciting thus far! Postbiotic substances include enzymes, bioactive peptides, short-chain fatty acids, antimicrobial peptides, polysaccharides, cell surface proteins, vitamins, plasmalogens, organic acids, and other compounds. Several studies demonstrate that short-chain fatty acids (SCFAs), in particular, reduce inflammation and improve the function of healthy lungs.9
Short-Chain Fatty Acids (SCFAs) and the Gut Microbiome-Lung Axis
Short-Chain Fatty Acids (SCFAs) include acetate, propionate, and butyrate and are primarily produced from dietary fiber by microbial fermentation.9,11 SCFAs play a role in many physiological processes, including the production of satiety hormones, energy expenditure, regulation of immune function, gut cell proliferation, and gut barrier function.9,12
A growing body of evidence demonstrates that SCFAs protect the lungs from infections by inhibiting the growth and virulence of infectious pathogens and modulating the immune response.13 We will not dive too deeply into how profoundly SCFAs affect immune function and reduce inflammation. However, ongoing research suggests SCFAs impact many different types of immune cells, including T regulatory cells, neutrophils, macrophages, dendritic cells, mast cells, effector CD4+ T cells, and B cells.11,14
Increase Short-Chain Fatty Acid (SCFA) & Postbiotic Levels to Reduce Inflammation
Fortunately, there are several ways to naturally support the health of the gut microbiome and increase postbiotic and SCFA levels. Since SCFAs are produced from the fermentation of dietary fiber, increasing dietary fiber intake could increase the production of SCFAs. The insufficient consumption of fiber-rich foods, such as fruits and vegetables, in Western countries may contribute to an increased prevalence of chronic disease due to the development of dysbiosis.9,13,14
Animal studies confirm a high-fiber diet increases circulating levels of SCFAs, decreases circulating levels of IgA, IgG, and IgE antibodies, reduces airway mucous production, alters gene expression, and provides protection against allergic inflammation in the lungs.9,13,14
Since the good bacteria in the gut microbiome ferment or transmute the dietary fiber into SCFAs, consuming more probiotics could also increase the production of SCFAs.15 The third option is taking supplemental SCFAs. Postbiotics, including SCFAs, are available as supplements. In animal studies, treatment with SCFAs replicated the protective effects of a high-fiber diet against allergic airway inflammation and inhibited the development of general airway hyper-reactivity.9
In additional animal studies, those treated with butyrate, a postbiotic SCFA, had lower levels of the inflammatory immune cells known as eosinophils, fewer inflammatory infiltrates, and less mucus production in the lungs.16
 Are Postbiotics & a Healthy Gut Microbiome-Lung Axis the Future of Asthma Treatment?
Are Postbiotics & a Healthy Gut Microbiome-Lung Axis the Future of Asthma Treatment?
Overall, the current research data suggest the gut microbiome-lung axis is characterized by a significant interplay between the gut microbiome and airway inflammation through the production of SCFAs and other postbiotic compounds. Future research will determine if healthy changes in the gut microbiome and/or supplementation with postbiotics could reduce the symptoms and severity of chronic asthma.13
Gut Microbiome Testing

To assess the health of the gut microbiome, screen for food sensitivities, measure levels of inflammatory markers, test for pathogens and opportunistic pathogens, and more, order our comprehensive Expanded GI Health Panel™ with GP3x and Calprotectin today.
- The Expanded Bacterial Stool Culture (GP3x) is a complete aerobic culture that reports all bacterial colonies isolated on the culture plates rather than the two or three most dominant species as reported on our standard (GP3) culture results.
- According to the American College of Gastroenterology clinical guidelines for the management of suspected IBS, a fecal Calprotectin test should be ordered as part of a comprehensive workup in all patients with gastrointestinal symptoms to rule out inflammatory bowel disease.
To place a test order, click here. As a reminder, DiagnosTechs will drop ship test kits directly to your patients. You may select this option at the top of the order form.
Please visit our Provider Tools page for the Complete GI Parasite List, Complete Yeast Culture List, and more information about choosing the right test, test result interpretation, treatment options, and more!
 References:
References:
- Hufnagl K, Pali-Schöll I, Roth-Walter F, et al. Dysbiosis of the gut and lung microbiome has a role in asthma. Semin Immunopathol. 2020;42(1):75-93. doi:10.1007/s00281-019-00775-y
- Jeyagurunathan A, Abdin E, Shafie S, et al. Asthma Prevalence and its Risk Factors Among a Multi-Ethnic Adult Population. Yale J Biol Med. 2021;94(3):417-427.
- Stern J, Pier J, Litonjua AA. Asthma epidemiology and risk factors. Semin Immunopathol. 2020;42(1):5-15. doi:10.1007/s00281-020-00785-1
- Khalaf K, Paoletti G, Puggioni F, et al. Asthma from immune pathogenesis to precision medicine. Semin Immunol. 2019;46:101294. doi:10.1016/j.smim.2019.101294
- Alwarith J, Kahleova H, Crosby L, et al. The role of nutrition in asthma prevention and treatment. Nutr Rev. 2020;78(11):928-938. doi:10.1093/nutrit/nuaa005
- Cresci GA, Bawden E. Gut Microbiome: What We Do and Don’t Know. Nutr Clin Pract. 2015;30(6):734-746. doi:10.1177/0884533615609899
- Kang YB, Cai Y, Zhang H. Gut microbiota and allergy/asthma: From pathogenesis to new therapeutic strategies. Allergol Immunopathol (Madr). 2017;45(3):305-309. doi:10.1016/j.aller.2016.08.004
- Chung KF. Airway microbial dysbiosis in asthmatic patients: A target for prevention and treatment?. J Allergy Clin Immunol. 2017;139(4):1071-1081. doi:10.1016/j.jaci.2017.02.004
- Chiu CJ, Huang MT. Asthma in the Precision Medicine Era: Biologics and Probiotics. Int J Mol Sci. 2021;22(9):4528. doi:10.3390/ijms22094528
- Salminen S, Collado MC, Endo A, et al. The International Scientific Association of Probiotics and Prebiotics (ISAPP) consensus statement on the definition and scope of postbiotics [published correction appears in Nat Rev Gastroenterol Hepatol. 2021 Jun 15;:]. Nat Rev Gastroenterol Hepatol. 2021;18(9):649-667. doi:10.1038/s41575-021-00440-6
- Föh B, Buhre JS, Lunding HB, et al. Microbial metabolite butyrate promotes induction of IL-10+IgM+ plasma cells. PLoS One. 2022;17(3):e0266071. doi:10.1371/journal.pone.0266071
- Salameh M, Burney Z, Mhaimeed N, et al. The role of gut microbiota in atopic asthma and allergy, implications in the understanding of disease pathogenesis. Scand J Immunol. 2020;91(3):e12855. doi: 10.1111/sji.12855
- Kim YJ, Womble JT, Gunsch CK, et al. The Gut/Lung Microbiome Axis in Obesity, Asthma, and Bariatric Surgery: A Literature Review. Obesity (Silver Spring). 2021;29(4):636-644. doi:10.1002/oby.23107
- Yip W, Hughes MR, Li Y, et al. Butyrate Shapes Immune Cell Fate and Function in Allergic Asthma. Front Immunol. 2021;12:628453. doi:10.3389/fimmu.2021.628453
- Machado MG, Sencio V, Trottein F. Short-Chain Fatty Acids as a Potential Treatment for Infections: a Closer Look at the Lungs. Infect Immun. 2021;89(9):e0018821. doi:10.1128/IAI.00188-21
- Vieira RS, Castoldi A, Basso PJ, et al. Butyrate Attenuates Lung Inflammation by Negatively Modulating Th9 Cells. Front Immunol. 2019;10:67. doi:10.3389/fimmu.2019.00067